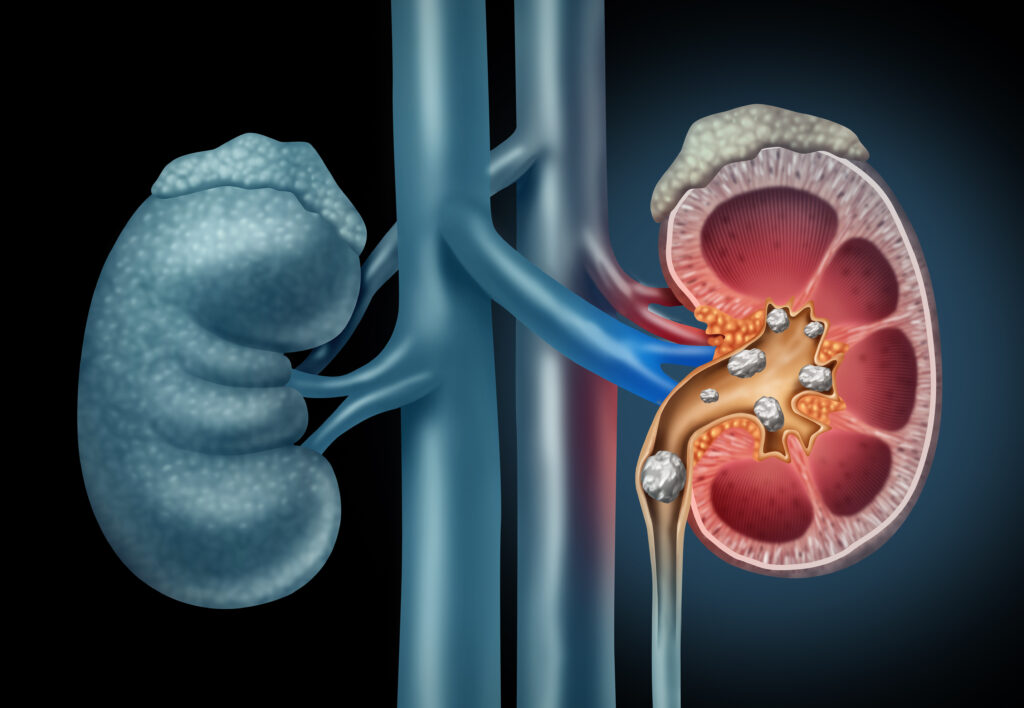
What Are Kidney Stones / Urinary Stones?
Your kidneys play a vital role in removing waste and excess water from your blood and turning it into urine. However, when there’s not enough fluid intake or too much of certain salts in the body, these substances can crystallize and start forming stone-like deposits in the kidneys.
These deposits may begin as tiny crystals, but over time, they can grow into larger stones. These are known as:

Kidney Stones

Urinary Stones

Renal Calculi

Nephrolithiasis / Urolithiasis
Once formed, these stones may:
- Remain in the kidney
- Or move into the urinary tract (ureter, bladder, or urethra)
This movement can cause urinary obstruction, pain, and even serious complications like infection or kidney failure if not treated on time, even if the stones are not currently causing pain.
Expert Stone Treatment with Dr Deval Parikh
He offer all globally recommended treatment options for kidney and urinary stones.
We understand that:
- Not all stones are the same
- And each patient may require a tailored treatment approach
Our team ensures that you receive the most effective and appropriate care for your specific type of stone.
What Are the Types of Kidney Stones / Urinary Stones?
Kidney stones can vary widely in size, shape, and texture, ranging from tiny particles like grains of sand to large stones as big as an egg. They may be smooth and rounded or rough with jagged edges, and each type is formed from different substances in the urine.
Based on their chemical composition, the five major types of kidney (or urinary) stones are:
- Calcium Oxalate Stones – The most common type, usually formed when there’s too much calcium and oxalate in the urine.
- Calcium Phosphate Stones – Often linked to metabolic conditions or certain medications that increase urinary calcium.
- Struvite Stones – Typically develop in response to urinary tract infections and can grow quickly and become quite large.
- Uric Acid Stones – More common in people who lose too much fluid, eat a high-protein diet, or have gout.
- Cystine Stones – Rare and usually hereditary, caused by a genetic disorder that results in excess cystine in the urine.
Understanding the type of stone is crucial for effective treatment and future prevention.
What Are the Risk Factors for Kidney Stones / Urinary Stones?
While anyone can develop kidney stones, certain factors significantly increase the risk. These include:
- Living in hot, humid climates or areas with hard water
- Low fluid intake over long periods, leading to concentrated urine
- Family history of kidney or urinary stones
- Recurrent urinary tract infections (UTIs)
- Excessive intake of:
- Calcium or uric acid
- Certain medications (e.g., diuretics, antacids)
- Vitamin D supplements
- Medical and metabolic conditions such as:
- Renal tubular acidosis
- Cystinuria
- Hyperparathyroidism
- Digestive disorders affecting nutrient absorption (e.g., Crohn’s disease)
- Renal tubular acidosis
Understanding these risk factors can help in preventing stone formation and choosing the right treatment options.
What Are the Symptoms of Kidney Stones / Urinary Stones?






💡 Important Note:
Not all kidney stones cause symptoms.
- Large stones may remain silent (asymptomatic) because they stay in one place and do not obstruct the flow of urine. These may go undetected for a long time, sometimes only discovered during tests for unrelated issues.
- On the other hand, small mobile stones or crystals traveling through the ureter (the tube from the kidney to the bladder) are often the cause of severe pain.
What Tests Are Required to Diagnose Stone Disease?
If a urinary stone is suspected, the doctor will first perform a clinical examination, followed by a series of tests to confirm the diagnosis and understand the location and impact of the stone. These typically include:
1. Initial Diagnostic Tests:
- Urine Examination – to check for infection, blood, or crystals
- Blood Test – to assess kidney function and detect abnormalities in calcium, uric acid, etc.
- Plain X-ray (KUB) – to detect radio-opaque stones (stones visible on X-ray)
- Ultrasound (Sonography) – to locate stones and assess the kidney and bladder condition
These tests are sufficient to diagnose stone disease in most patients.
2. Advanced Imaging (if needed):
- CT Scan (Non-contrast Spiral CT or CT KUB) – provides detailed imaging to detect even very small stones
- Intravenous Urography (IVU) or CT Urogram – used when interventional treatment is planned. In this test, a contrast dye is injected into a vein, and a series of X-rays or scans are taken to:
- Visualize the function of each kidney
- Understand the detailed anatomy of the urinary tract
These advanced tests help in planning the most suitable treatment approach, especially in complex or recurring cases.
Do All Kidney Stones/Urinary Stones Require Treatment?
No, not all kidney or urinary stones require interventional treatment. Many small stones can pass naturally through the urinary tract without causing damage.
When Can Stones Pass on Their Own?
- In over 60% of cases, stones smaller than 6 mm pass out spontaneously
- These cases are managed with conservative treatment, such as:
- Increased fluid intake
- Pain relief medications
- Specific medications to help stone passage
When Is Interventional Treatment Needed?
Treatment is usually necessary when:
- The stone is too large to pass naturally
- There are severe symptoms (e.g., intense pain, nausea)
- There’s a significant urinary blockage or infection
- The stone is associated with abnormalities in the urinary tract anatomy
- The stone is causing damage to the kidney
What Are the Treatment Options for Kidney Stones / Urinary Stones?
Treatment options for kidney (urinary) stones range from conservative (non-surgical) to interventional (surgical), depending on the size, location, symptoms, and risk of complications.
1. Conservative Management (Non-Surgical Treatment)
This is a wait-and-watch approach and is recommended when:
- The stone has a high chance of passing naturally
- It is not causing significant symptoms or complications
- The risk of damage to the kidney or urinary tract is low
What it includes:
- Adequate hydration
- Medications to:
- Help dissolve certain types of stones
- Treat infection (if present)
- Relieve pain
Ease the passage of the stone
2. Interventional Treatment (Surgical or Procedural)
This is advised when:
- The stone is too large, oddly shaped, or unlikely to pass naturally
- The stone causes severe symptoms, infection, or blocks the urine flow
- There are anatomical abnormalities
- Stones are present on both sides (bilateral) or causing recurring problems
Types of Interventional Treatments:
1. Non-Invasive:
- Shock Wave Lithotripsy (SWL): Uses sound waves to break the stone into tiny pieces
- RIRS (Retrograde Intrarenal Surgery): A flexible scope enters the kidney via the urethra to remove/break stones
- Ureteroscopy: A thin scope is passed through the urinary tract to remove or break stones
2. Minimally Invasive:
- PCNL (Percutaneous Nephrolithotomy): Small incision in the back to remove large or complex stones
3. Invasive:
- Open Stone Surgery: Rarely used today, for very large or complicated stones when other methods aren’t suitable
Kidney Stone Treatment Options
Treatment depends on the stone’s size, location, hardness, and the patient’s condition. Here’s an overview of the six main options available:
1. Shock Wave Lithotripsy (E.S.W.L.)
Type: Non-invasive
Best for: Small, soft stones in the kidney or upper ureter
Procedure:
- No cuts or surgery needed
- You lie on a table; an anesthetic cream is applied
- X-ray guides the machine to target the stone
- Shock waves are sent to break the stone into tiny particles
Recovery:
- Outpatient procedure; no hospital stay
- Resume work the next day
- Stone fragments pass naturally over the next few days
- Follow-up X-ray after 3 weeks
❗ Not ideal for large/hard stones—may need multiple sittings or alternate treatments like RIRS or PCNL
2. Ureteroscopy (U.R.S.)
Type: Endoscopic (minimally invasive)
Best for: Stones in the ureter
Procedure:
- Under anesthesia, a telescope-like device is passed through the urinary tract to reach the stone
- The stone is either removed whole or broken using laser/pneumatic energy
- A stent may be placed and removed later
Recovery:
- 1–2 day hospital stay
- Resume normal routine in a few days
- Follow-up imaging confirms complete clearance
Globally preferred for ureteric stones. Highly effective and almost painless.
3. Retrograde IntraRenal Surgery (R.I.R.S.)
Type: Advanced endoscopic
Best for: Stones inside the kidney (even hard stones)
Procedure:
- Done under general anesthesia
- A flexible scope is inserted through the urinary tract up into the kidney
- Stones are fragmented and removed
- A stent may be placed temporarily
Recovery:
- 1–2 day hospital stay
- No body cuts or blood loss
- Resume routine activities the next day
- Safe for diabetics and patients on blood thinners
Follow-up in 3 weeks with a check X-ray
4. Percutaneous Nephrolithotomy (P.C.N.L.)
Type: Minimally invasive
Best for: Large, hard, or multiple kidney stones
Procedure:
- Under anesthesia, a small incision is made in the back
- A tract is created to access the kidney using a scope
- Stones are broken and removed through suction or tools
- A stent may be placed temporarily
Recovery:
- 4–7 day hospital stay
- Avoid heavy work for 4–6 weeks
- Follow-up imaging after 2 days
💡 Especially useful for stones that cannot be treated with ESWL or RIRS
5. Laparoscopic Treatment
Type: Minimally invasive surgery
Best for: Rare, complex cases not suitable for endoscopic methods
Why it’s less preferred:
- Requires multiple small cuts and general anesthesia
- Longer surgery and recovery time
Higher risk compared to endoscopic procedures
6. Open Stone Surgery
Type: Traditional major surgery
Best for: Rare or very complex situations only
Why it’s outdated:
- Large incision, painful, longer hospital stay
- High recovery time and visible scar
- Risky if future surgery is needed
